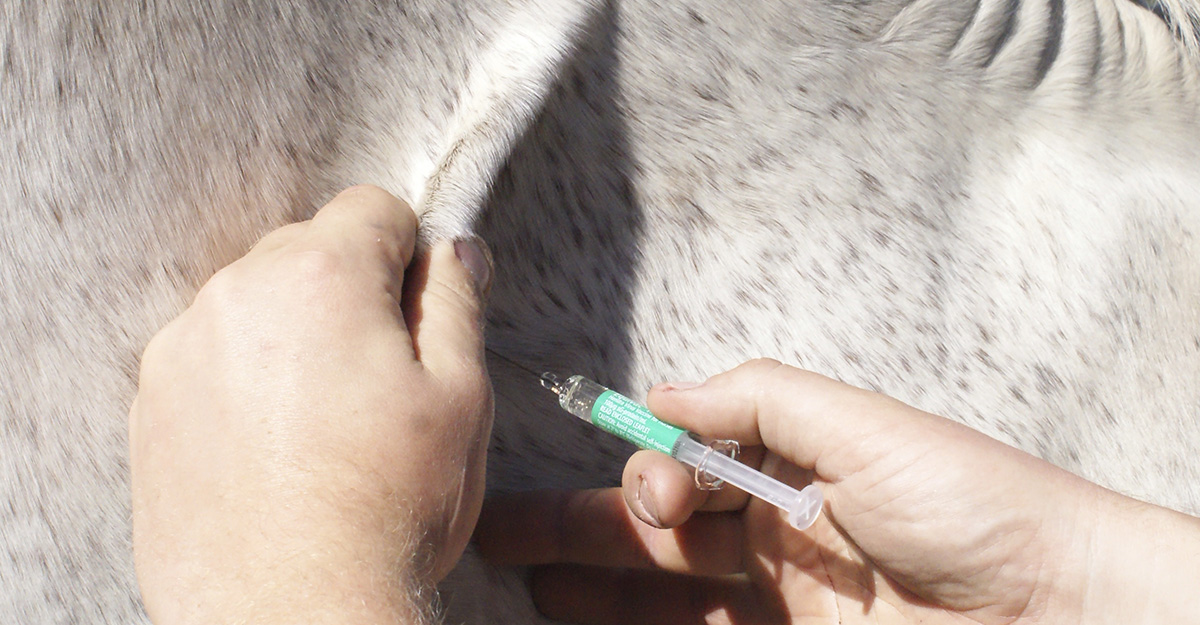
The mantra that prevention is better than cure is recited so often these days that it is fast becoming a cliché. It is true though, and vaccination is probably the cardinal example of this.
By priming your horse’s immune system before it is exposed to a disease, it will have the capacity to respond rapidly, multiplying antibody-producing white blood cells that will attack, capture and rid the body of the particles that cause disease and winning the arms race.
But while vaccines are routinely administered all around the world, there is still a fair amount of skepticism about their safety, and confusion about their side effects. In this article, Dr Euan Laidlaw explains the science behind vaccines and how they help protect, not just your horse, but the horse industry, the economy at large, and in some cases, human health.
Vaccination against various diseases must be one of the most common equine veterinary procedures, certainly in the developed world and, as an ambulatory vet, it’s something I do almost every day. The frequency and, in most cases, ease with which this is practiced can lead to complacency with regard to its importance and certainly doesn’t do justice to the complexity of the science behind it – something which has been baffling and bewildering veterinary students for centuries!
Scroll down to read about the common diseases we can vaccinate horses against.
So, how did it all start? The father of vaccination – human and animal – as we know it today was an Englishman, Edward Jenner who, in 1796, conscripted his gardener’s son for an experiment.
Jenner took the pus from cowpox blisters on some affected cattle and smeared it on both arms of eight-year-old James Phipps; resulting in some irritation and a mild fever, which passed in a few days.
Sometime later, Jenner then injected Master Phipps with human smallpox; a frequently fatal disease. Phipps had no symptoms. Jenner repeated this multiple times to great success. This worked because the two viruses in question – cowpox and smallpox – can both infect humans and are very similar in their outer microscopic structure.
It is this outer structure, known as an antigen, of the virus particles that the immune system of all mammals recognises and produces specific killer substances (antibodies) against. Having seen cowpox and successfully fought off that infection, some cells with the ability to produce these specific killer antibodies against pox were retained.
On subsequent exposure to similar smallpox, these primed cells were able to multiply rapidly and quash the infection, which may have been fatal in an immune-naïve individual. This represents what we call ‘active immunity’; where the body becomes immune to a disease as a result of previous exposure to it – or indeed, a vaccination which mimics its structure.
This is also an example of use of a live vaccine; where there is a risk of disease. Nowadays, these have been largely replaced by more modern technology, where we use only part of the particle in a vaccination. This allows the immune system to learn how to kill the real thing, but the vaccine, in itself, is not capable of causing serious harm.
In moving from live vaccination to our less risky modern equivalents – which contain dead disease particles or, in some cases, just a single or multiple parts of these – we have had to add immune stimulants to the mixture in the syringe. These are known as adjuvants. They are usually fairly inert substances, such as aluminium phosphate or mineral oil. They serve as a flag to the immune system, alerting white blood cells to the fact a vet has just given the horse a vaccine.
Whilst making our vaccines much more effective, it is often these adjuvants which are responsible for creating common vaccination reactions. Many horse people will know of one which has had a swelling at the injection site after its vaccination.
These are seldom serious and usually subside in a few days. Some horses, just like humans, will feel a bit average for a day or two after a vaccination. This is due to a temporary, mild fever they experience. Again, this is uncommon and seldom a cause for concern if treated appropriately by your vet.
So far, we’ve been discussing active immunity. The other equally important branch of the immune system is known as passive immunity. This is where instead of an animal making its own antibodies (substances to kill disease with), it receives them pre-formed.
The two main instances of this in a horse’s life occur at birth; where a newborn foal drinks colostrum and when a vet administers tetanus antisera following a wound.
A newborn foal is completely immune naïve, having had no history of exposure to bacteria, viruses and other disease-causing bugs and, therefore, is at high risk! Nature’s mechanism of protection for this cute character is its dam’s first colostrum-rich milk. Colostrum is packed full of not only nutrition, but immunity. And, for this reason, it is essential that your Bambi-on-ice finds his or her feet quickly and ingests plenty in the first few hours of life.
The gut of a newborn foal starts like a sieve, with big holes allowing these antibodies that provide protection to move straight into the blood stream. As the hours tick by, the holes in the sieve close up to the point that antibodies are no longer allowed through. This gradual closure is as good as complete come 24 hours since birth and what the foal then has is its entire immune system for the first few months of life.
I encourage all breeders to have a blood test taken at this point to assess the level of success of this passive transfer of immunity. This is quick and cheap, and should the result be the foal hasn’t received enough for whatever reason, it can be topped up before any infection gets a chance to take hold.
This is done by a plasma transfusion, where some commercially harvested plasma (blood that has had the red and white cells removed) is given to the foal via an intravenous drip. The blood used to make the plasma is taken from mares kept specifically for the purpose. These horses are given extra vaccines prior to donating, meaning their levels of antibodies are far higher than a normal non-vaccinated horse.
Another common way in which our equines receive passive immunity is through tetanus anti-toxin. Tetanus bacteria can be found in soil, where they can lie dormant for years in a form known as ‘spores’. Given the correct conditions, i.e. a dirty wound, these spores can change form to one which produces a toxin that, in turn, attacks the nervous system of the horse. This produces the disease we recognise as tetanus, where horses become stiffer and stiffer until they are spastically paralysed with all their muscles trying to contract simultaneously. It’s a truly horrible disease that’s often fatal.
This can be prevented or treated using hyperimmune antisera, produced by first intensively vaccinating adult horses, then taking some of their blood, from which the necessary components are purified and packaged, ready to be administered to a newborn foal, an unvaccinated horse potentially facing a challenge or to try to treat a horse suffering from tetanus.
Vaccination requirements vary depending on a large number of factors, including the country, animal, holding and purpose to name but a few. Common vaccination protocols in Australia currently include tetanus, strangles, Hendra and, in some cases, herpes.
In the United Kingdom, we routinely vaccinate against tetanus, flu and, in some cases, herpes. Whatever your individual horse’s situation, I encourage you to ask your vet which vaccinations they recommend and follow their guidance. This can be done with the peace of mind that over-vaccination is not something we recognise as causing a problem from an animal health perspective; even if it is from a cynical journalism point of view.
The mantra that prevention is better than cure is recited so often these days that it is fast becoming a cliché. It is true though and vaccination is probably the cardinal example of this. By priming your horse’s immune system before it is exposed to a disease, it will have the capacity to respond rapidly, multiplying antibody-producing white blood cells that will attack, capture and rid the body of the particles that cause disease and winning the arms race.
This is far preferable to letting the bacteria or virus spread rapidly through the body, as it will do if the immune system is too slow. Once disease has set in, your vet will have to reach for other drugs, like antibiotics – which due to the growing bacterial resistance, we’re trying to reserve for when humans get ill.
Common diseases
TETANUS
Tetanus, or clostridium tetani, is a bacterial infection that causes death in about 80% of horses that become infected. Horses can become infected at any age. The organism which causes the disease lives in manure and soil, and infects wounds and deep cuts where oxygen is poor. From one-three weeks after being infected, horses can start to show signs of progressive muscle cramping. Death can occur within a few days of the first signs. The first signs can be an abnormal gait, resting stance (sawhorse) or abnorma behavior, which can include erect ears and stiffness to the facial muscles and legs. A number of the body’s muscles then go into spasms, including the spasm of the third eyelid. Treatment includes intense nursing care with sedatives, antibiotics, muscle relaxants, anti-toxin and, in many cases, tube feeding the horse as it is unable to eat. Vaccinating against Tetanus should be started in foals at the age of 12 weeks if the mare has been vaccinated prior to foaling. If the mare has not been vaccinated, an initial vaccination of tetanus antitoxin should be given at birth or after injury, which will give short term protection – three weeks approximately – and a booster four months later. Boosters are suggested to be given every year when you vaccinate against strangles, often called the 2-in-1.
EQUINE INFLUENZA
Equine Influenza (EI) is a highly contagious, viral disease affecting all equine species. It causes a sudden increase in temperature, with a deep, dry, hacking cough and a watery nasal discharge that can become thick, smelly and green/yellow. Horses can become depressed, show muscle pain and stiffness, and have laboured breathing. Being highly contagious, the transmission of the EI virus from horse to horse can be done through direct contact from an infected horse, contact with contaminated tack or equipment, contact with a horse handler that has previously handled an infected horse, or indirect contact with infected buildings or floats.
This disease is not generally fatal to horses, but the aged, very young or sick may have further problems stemming from the initial disease, such as bronchopneumonia or bronchitis. Horses that are affected need to be rested and isolated for as long as their coughing remains. Recovery usually occurs after a couple of weeks from the onset of signs and veterinary attention is not normally sort unless the horse is showing other signs. In Australia, horses are not vaccinated against EI as it is a disease not seen in Australia.
In August 2007, Equine Influenza escaped from the Easter Creek Quarantine Station in Sydney. The outbreak that eventuated was the most serious emergency animal disease Australia has experienced in recent history. At its peak, 47,000 horses were infected in NSW on 5943 properties, and horse owners and industry workers were facing dark times with major impacts on their livelihood and lifestyle. The campaign led by NSW DPI to eradicate the disease was the largest of its type ever undertaken in Australia, using the latest laboratory, vaccine, surveillance, mapping and communication technologies.
The disease was eradicated in Australia within six months well ahead of predictions and by July 2008 horse industry operations had returned to normal.
EQUINE HERPES VIRUS
Rhinopneumonitis or equine Herpes is a common virus that occurs worldwide in horse populated areas. There are nine different herpes viruses that are recognized (EHV-1 to EHV-9), but the two most common strains are EHV-1, which causes respiratory disease, abortions and neurological disease, and the EHV-4, which causes respiratory disease and the occasional abortion. Respiratory disease caused by EHV is more common in foals and yearlings, and older horses are more likely than younger ones to transmit the virus without showing any signs.
One-two days after exposure, the onset of respiratory or neurological disease begins with a fever, and abortion syndrome can occur up to four months later. Horses can shed the virus from the nasal passages when they cough or snort for a further two-three weeks after clinical signs start. Any horse showing signs should be isolated immediately for up to four weeks. Affected horses show weakness and incoordination and, sometimes, are unable to get up after lying down.
Most clinical signs will stabilie and begin to improve within hours. However, some horses can continue to deteriorate, and may take weeks or months to fully recover. These clinical signs are due to infection of the blood vessels within the neurological system, usually within the spinal cord.
In the last trimester (8-11 months), pregnant mares abort as the EHV-1 results in infection of the blood vessels of the placenta. The result of the infection makes the placenta detach. All aborted material should be disposed of immediately as this is infected and can infect other pregnant mares. The mare should be isolated as well. There is no specific treatment for herpes virus except for supportive care with antibiotics and antinflammatories. Vaccination should start at 13 weeks of age with two doses four weeks apart.If not vaccinated, one dose every six months or, if in foal, one dose at five, seven and nine months of gestation.
An EHV-1 outbreak during a showjumping event in 2021 led to the death of 18 elite competition horses and the cancellation of national and international horse events in 12 countries.
STRANGLES
Strangles, or Streptococcus Equi, is an upper respiratory disease that affects the lymph nodes of the horse’s head. The organism spreads rapidly from horse to horse through coughing, or from eating or drinking infected droplets. These droplets may remain infective for over a month in the right conditions. It takes three-eight days after becoming infected for a horse to show signs.
A fever from 39.5-40.5C will show, followed by the throat and larynx becoming inflamed, and drinking or swallowing food becomes difficult and painful. The lymph nodes of the head become very swollen and painful and, with time, may burst and discharge thick purulent discharge. Sometimes, the infection can spread to other parts of the body and this is called ‘bastard strangles’. This form is very difficult to treat and sometimes cannot be treated at all.
When a horse is infected, treatment is symptomatic. Isolating the horse, using antibiotics and supportive nursing care, plus cleaning and disinfecting all water, feed buckets, grooming and saddlery equipment, stables, etc. will help stop the transmission to other horses. Strangles can still occur in horses that are vaccinated, so regular boosters are required to provide protection. Foals are to start their vaccination program at 12 weeks of age, with a booster every two weeks for three doses then yearly.
Owners with horses older than 12 months of age who have never been vaccinated or broodmares, should consult their local large animal vet for vaccination instructions.
AFRICAN HORSE SICKNESS
African horse sickness (AHS) is a highly infectious and deadly disease caused by African horse sickness virus. It commonly affects horses, mules, and donkeys. It is caused by a virus of the genus Orbivirus belonging to the family Reoviridae. This disease can be caused by any of the nine serotypes of this virus.
AHS is not directly contagious, but is known to be spread by insect vectors. AHS is known to be endemic in sub-Saharan Africa, and has spread to Morocco, the Middle East, India, and Pakistan. More recently, outbreaks have been reported in the Iberian Peninsula (1987-1990) and Thailand (2020). AHS has never been reported in the Americas, eastern Asia, or Australasia. Epidemiology is dependent on host-vector interaction, where cyclic disease outbreaks coincide with high numbers of competent vectors.
The most important vector for AHS in endemic areas is the biting midge Culicoides imicola, which prefers warm, humid conditions. Larvae do not carry the virus, and long, cold winters are sufficient to break epidemics in nonendemic areas. Horses are the most susceptible host with a mortality rate of 50% to 95% of those affected, followed by mules (50%) and donkeys (5-10%). In African donkeys and zebras mortality is rare. They very rarely display clinical symptoms, despite high virus titres in blood and are thought to be the natural reservoir of the virus.
According to the OIE, at present, only the live attenuated AHS vaccines currently exist – a polyvalent vaccine, a monovalent vaccine. There was a monovalent inactivated vaccine, but it is no longer available. A serotype specific subunit vaccine is currently in development. While it might seem paradoxical, AHS vaccination itself presents a risk. The live attenuated virus used in vaccines has been known to replicate and create its own, albeit less severe, form of outbreak.
Early in 2020, African Horse Sickness (AHS) ferociously killed hundreds of Thai horses in less than three weeks in an outbreak that purportedly started after zebras were imported from Africa. Australia has strong biosecurity protocols to prevent AHS from entering its borders, such as only permitting imports from countries that have been free from AHS for two years prior to export and which do not allow vaccination.
SALMONELLA
There are many Salmonella bacteria that can affect any animal, but the most prevalent one to affect horses is S.Typhimurium. In adult horses, the Salmonella bacteria can cause gastrointestinal disease which leads to severe diarrhoea and, in some cases, usually in foals, it can cause septicemia. Salmonella can also affect the kidneys, liver, heart, laminitis and weight loss. Very rarely can it cause abortion in mares. Salmonella is transmitted by the ingestion of contaminated faecal material. The bacteria are shed in the manure of infected horses and then ingested by other horses by eating the grass, hay or other infected material. It can also be passed on by the footwear of horse owners, grooming brushes, and water or feed buckets. Once infected, adult horses develop a high temperature with severe foul smelling, watery diarrhoea. Sometimes, there can be blood in the manure. Foals that are septic with Salmonella are found to be lethargic and depressed with a high temperature. They are sometimes lame with swollen joints. Death can occur if diarrhoea is persistent. Many horse carry the bacteria in their system, but do not shed it or show any signs of the disease. Salmonella is a zoonotic disease, meaning it can be passed to humans, so using good hygiene practices can help with keeping the transfer to a minimum. Treatment is systematic, involving fluid therapy and antinflammatories. Research shows the risk of Salmonella is increased in horses fed feeds that are fermented in the hindgut (caecum). Vaccinating should start at three months of age with two doses one month apart. For breeding mares, the same applies if the vaccinating history is unknown – two doses one month apart. For mares already vaccinated, a booster should be given one month prior to foaling every year.
EQUINE ROTAVIRUS
Rotavirus is a major cause of infectious diarrhoea in foals and can be the cause of 50-90% of foal diarrhoea. Foals are more susceptible to this virus due to an underdeveloped immune system and it can affect them from one week to five months of age. While Rotavirus morbidity can be as high as 50%, mortality is as low as 1% if immediately treated by a veterinarian. Rotavirus is transferred from faeces to mouth, and usually results in damage to the small intestinal absorption capabilities, causing watery diarrhoea. Most foals that develop diarrhoea will not require veterinary attention. However, some can get quickly dehydrated and require fluids. As many as 70% of foals will have a bout of diarrhoea at some stage before weaning and many owners commonly mistake this for hormonal changes in the mare when, in actual fact, it may be caused by the rotavirus. Any foal showing signs of diarrhoea should be isolated from any other horses and treated as infectious. All breeding mares should receive a vaccination at eight, nine and 10 months of pregnancy. A booster should be given one month prior to foaling in each subsequent pregnancy. Following the vaccination guidelines will help stimulate the production of antibodies in the colostum and milk against the rotavirus. Adult non-breeding horses do not need to be vaccinated.
HENDRA VIRUS
Hendra virus (HeV) is a zoonotic disease (can pass from animals to humans) that is carried by flying foxes and can pass to horses and then on to humans. Whilst the likelihood of horses or humans contracting the disease remains very low, it can produce life-threatening illness, which has no cure or specific treatment.
The virus was first identified in 1994 and the testing protocol has detected Hendra Virus in Eastern Australia on 62 occasions causing the death or euthanasia of more than 100 horses, two dogs and four people, with a further three human cases who survived the disease.
HeV is a notifiable disease and is found exclusively in Australia. A close relation, the Nipah virus, has been found in Asia.
The incubation period for HeV, from infection to onset of symptoms may vary between 5 to 16 days, and onset is sudden, with rapid deterioration. Signs vary from case to case, as the virus can affect different parts of the body, but includes fever, depression, lethargy, increased heart rate, laboured breathing, frothy nasal discharge, discomfort/weight-shifting between legs, sweating, muscle weakness, spasms or twitching, wobbly gait, balance difficulties, weakness, lethargy, circling, loss of coordination, head-pressing, convulsions and collapse, urinary incontinence and colic. Death usually occurs within 48 hours. HeV should be considered with the sudden death of an otherwise healthy horse.
The disease is only transmitted to people through very close contact with secretions or bodily fluids of infected horses. An infected horse can excrete HeV through nasal discharges for up to 72 hours before clinical signs appear, mortality is 70% and diagnosis is based on veterinary blood tests and swabs.
Vaccination of horses is crucial to break the cycle of HeV transmission from flying foxes to horses and then to people, as it prevents both the horse developing the disease and passing it on. It also protects horses from shedding the virus.
In 2021, a new strain of Hendra virus was identified as the cause of death of a horse that died in South Australia in 2015. The testing protocols at the time were only capable of detecting the strain of the virus that is carried by the Black Flying Fox commonly found in Northern Australia, but new testing protocols have been developed to identify a second strain of the virus, one which has been found in 2013 in a Grey Headed Flying Fox, of the species that live in coastal areas of Eastern Australia, from Rockhampton to South Australia.